FOOD POISONING REMEDY TIPS
March 26, 2022Diabetes mellitus is a metabolic disorder characterized by excessive amount of glucose in the bloodstream or chronic hyperglycemia. Uncontrolled diabetes is a major cause of kidney failure, blindness, amputation, and increases risk of heart attack and stroke.
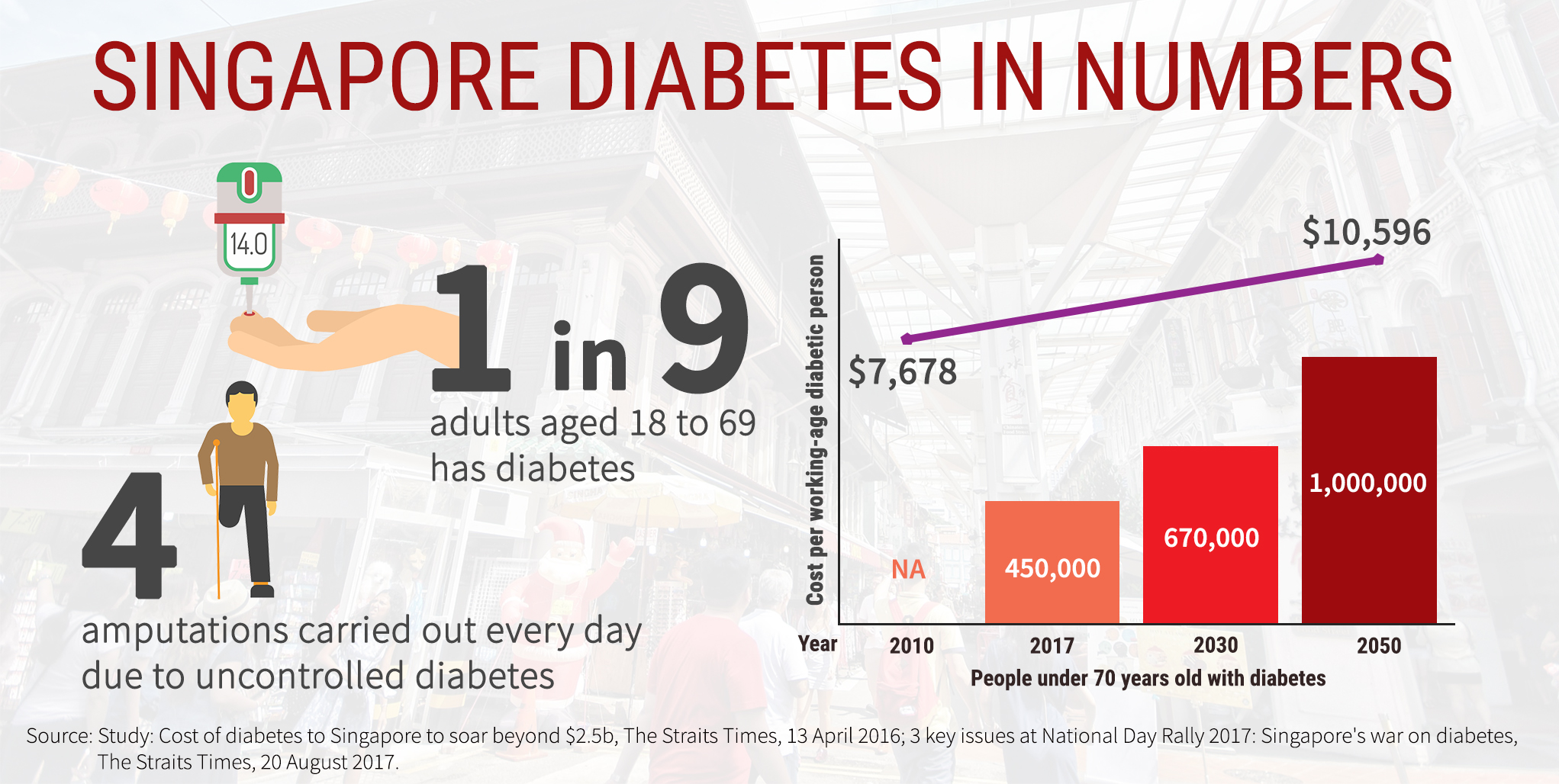
In Singapore every day, 4 amputations are the results of uncontrolled diabetes.
The average cost per working-age diabetic person was $7,678 in 2010. This number is forecast to go up to $10,596 by 2050, with indirect costs rising to account for 65 per cent of this figure.
In 2017, there were more than 450,000 Singapore residence with diabetes. This number is predicted to rise to 670,000 in 2030 and 1,000,000 in 2050.
Over 90% of diabetic individuals in Singapore belong to type 2 diabetes, a condition when the body does not properly utilise insulin or insulin resistance. Type 2 diabetes is usually related to sedentary lifestyle and poor eating habit.
Type 2 diabetes is preventable. And, yes, you can reverse type 2 diabetes
There are three types of diabetes: type 1 diabetes, type 2 diabetes, and gestational diabetes that occurs during pregnancy.
Type 1 diabetes occurs when damaged pancreas does not produce insulin – a hormone produced by pancreas to break down sugar in the bloodstream and keep blood sugar level balanced. Type 1 diabetes is an autoimmune condition caused by the body attacking its own pancreas with antibodies. Its dominant predisposing factor is genetic and cannot be prevented. It usually occurs in young people. Individuals with type 1 diabetes need insulin injections to control their blood glucose level.
Type 2 diabetes occurs when pancreas does not produce sufficient insulin and/or the body does not respond properly to insulin. Lack of sensitivity to insulin otherwise known as insulin resistance, happens primarily in fat, liver, and muscle cells. By far, type 2 diabetes is the most common form of diabetes prevalence worldwide. Type 2 diabetes can be prevented, and the disease can be reversed.
Gestational diabetes develops when high blood sugar levels in a mother are circulated through the placenta to the baby. It is an insulin resistance triggered during pregnancy, in the middle to late stage. If not controlled, gestational diabetes may affect baby’s growth and development. Gestational diabetes usually resolves itself after pregnancy, however, it heightens the risk of mothers developing type 2 diabetes later in life.

The human gastrointestinal tract is a complex and dynamic ecosystem referred to as the gut microbiome. It contains in average 100 trillion of symbiotic microorganisms, and features over 5,000 bacterial species.1
The relationship between the gut microbiome and human health is becoming increasingly recognised. It is now well-established that a healthy gut microbiome plays pivotal roles in maintaining in human health such as immune system maturation, metabolism of glucose, lipids, and bile acids, defence against pathogens, increase nutrient uptake, and activating immune system.2
On the other hand, imbalanced composition of these commensal microbiota or dysbiosis, is closely associated with conditions such as celiac disease, inflammatory bowel disease (IBD), and irritable bowel syndrome (IBS), obesity, pancreatitis, diabetes, hypertension, cardiovascular diseases, dyslipidaemia, and cancer.3,4
In type 2 diabetic individuals, not only are their bacterial compositions different from healthy subjects, but chronic low-grade inflammation in the different tissues have been linked as contributory factors in insulin resistance.5
Probiotics (live beneficial bacteria) and postbiotics (secondary metabolites produced by probiotics) are able to confer beneficial effects by balancing and restoration of the gut microbiome, protection against pathogens, anti-inflammatory effects, immunomodulatory effects, antioxidative effects, and maintenance of intestinal barrier integrity.6
Increasing evidence has demonstrated that probiotics and postbiotics could reduce fasting blood glucose, insulin levels, improve glycosylated haemoglobin (HbA1c) and insulin resistance, improve metabolic and inflammatory status of diabetic individuals, supporting the importance of gut health in management and reversal of type 2 diabetes.7,8,9
Together with probiotics or postbiotic supplementation, we strongly advocate having a balanced lifestyle: regular exercise, healthy diet, and weight management as part of holistic approach not just in beating type 2 diabetes, but also in maintaining a healthy gut and overall health.
- Aline Corado Gomes, Allain Amador Bueno, Rávila Graziany Machado de Souza and João Felipe Mota: Gut microbiota, probiotics and diabetes. Gomes et al. Nutrition Journal 2014, 13:60.
- Annalisa Noce, Giulia Marrone, Francesca Di Daniele, Eleonora Ottaviani,Georgia Wilson Jones, Roberta Bernini, Annalisa Romani and Valentina Rovella: Impact of Gut Microbiota Composition on Onset and Progression of Chronic Non-Communicable Diseases. Nutrients 2019, 11, 1073.
- D. Pagliari, A. Saviano, E. E. Newton, M. L. Serricchio, A. A. Dal Lago, A. Gasbarrini , and R. Cianci: Review Article – Gut Microbiota-Immune System Crosstalk and Pancreatic Disorders. Hindawi Mediators of Inflammation Volume 2018, Article ID 7946431.
- José E. Belizário, Joel Faintuch, and Miguel Garay-Malpartida: Review Article – Gut Microbiome Dysbiosis and Immunometabolism: New Frontiers for Treatment of Metabolic Diseases. Hindawi Mediators of Inflammation Volume 2018, Article ID 2037838.
- Nathalie M. Delzenne1 & Patrice D. Cani & Amandine Everard & Audrey M. Neyrinck & Laure B. Bindels: Gut microorganisms as promising targets for the management of type 2 diabetes. Diabetologia (2015) 58:2206–2217.
- Núria Piqué , Mercedes Berlanga and David Miñana-Galbis: Health Benefits of Heat-Killed (Tyndallized) Probiotics: An Overview. Int. J. Mol. Sci. 2019, 20, 2534.
- Qingqing Zhang, Yucheng Wub, Xiaoqiang Fei: Effect of probiotics on glucose metabolism in patients with type 2 diabetes mellitus: A meta-analysis of randomized controlled trials. MEDICINA 52 (2016) 28–34.
- Neel Jayesh Shah, Onkar C. Swami: Role of Probiotics in Diabetes: A Review of Their Rationale and Efficacy. EMJ Diabet. 2017;5[1]:104-110.
- Alessandra Puddu, Roberta Sanguineti, Fabrizio Montecucco, and Giorgio Luciano Viviani: Review Article – Evidence for the Gut Microbiota Short-Chain Fatty Acids as Key Pathophysiological Molecules Improving Diabetes. Hindawi Publishing Corporation Mediators of Inflammation Volume 2014, Article ID 162021.
Most scientific reference of probiotics and postbiotics are done on Lactobacillus genus, whose long history of use in fermented products has led to their recognition as GRAS (Generally Recognized As Safe) by the US Food and Drug Authority (FDA), and earned them a place on the QPS (Qualified Presumption of Safety) list assembled by the European Food Safety Authority (EFSA).